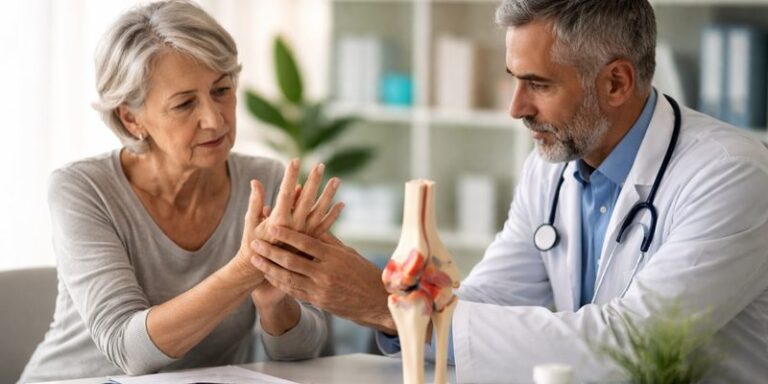
Arthritis is not a single disease but a broad term used to describe conditions that affect the joints, surrounding tissues and, in some cases, other parts of the body. It is one of the most common causes of pain, stiffness and reduced mobility worldwide. Although arthritis is often associated with older people, it can affect adults of any age and, in some forms, even children. The two best-known types are osteoarthritis, which involves the gradual breakdown of joint cartilage, and rheumatoid arthritis, an autoimmune condition in which the immune system attacks the lining of the joints (NHS, 2023; Smolen et al., 2016).
Arthritis can have a major impact on everyday life, making walking, dressing, climbing stairs and working more difficult. However, early diagnosis, healthy lifestyle choices and appropriate treatment can help many people manage symptoms well and maintain independence. This article discusses the causes, symptoms, prevention and management of arthritis, with examples from common forms of the condition.
1.0 Understanding Arthritis
1.1 What is Arthritis?
Arthritis refers to inflammation, degeneration or damage affecting one or more joints. Joints such as the knees, hips, hands and spine are often involved because they are used repeatedly and bear weight. In osteoarthritis, cartilage becomes thinner and the joint changes over time, leading to pain and stiffness. In rheumatoid arthritis, inflammation can damage joints and may also affect the eyes, lungs and blood vessels if it is not controlled (Hunter and Bierma-Zeinstra, 2019; Kumar and Clark, 2020).
1.2 Common Types
The most common forms include:
1.2.1 Osteoarthritis
This is the most prevalent type. It is linked with ageing, joint overuse, previous injury and obesity. For example, a former footballer with repeated knee injuries may develop osteoarthritis earlier than expected because of long-term joint stress.
1.2.2 Rheumatoid Arthritis
This is an autoimmune disease. The immune system mistakenly attacks the synovium, the lining of the joints, causing swelling, pain and, eventually, joint damage. It often affects the small joints of the hands and feet symmetrically, meaning both sides of the body are involved (Smolen et al., 2016).
Other forms include gout, caused by uric acid crystal deposition, and psoriatic arthritis, which may occur in people with psoriasis (McInnes and Schett, 2017).
3.0 Causes and Risk Factors
3.1 Age and Wear and Tear
Age is a major factor, especially in osteoarthritis. Over time, repeated movement and loading can lead to gradual cartilage deterioration. This does not mean arthritis is simply an inevitable part of ageing, but the risk does increase with age (Hunter and Bierma-Zeinstra, 2019).
3.2 Genetics
Some people inherit a greater tendency to develop certain forms of arthritis. A family history of rheumatoid arthritis, for instance, can raise risk, especially when combined with environmental triggers such as smoking (Smolen et al., 2016).
3.3 Excess Weight
Obesity is strongly linked with osteoarthritis, particularly of the knees and hips. Extra body weight increases mechanical pressure on joints and may also promote low-grade inflammation in the body (NICE, 2022). For example, someone who is significantly overweight may notice knee pain worsening after standing or walking for long periods.
3.4 Joint Injury and Occupation
Previous injuries, heavy lifting and repetitive movements can damage joints over time. Jobs involving kneeling, squatting or frequent manual labour may contribute to osteoarthritis in susceptible individuals.
3.5 Immune and Metabolic Factors
Rheumatoid arthritis is caused by immune system dysfunction, while gout develops when uric acid levels become too high. Diet, kidney function, alcohol intake and some medicines can influence gout risk (National Institute of Arthritis and Musculoskeletal and Skin Diseases, 2023).
4.0 Symptoms of Arthritis
4.1 Joint Pain and Stiffness
The hallmark symptoms are pain, stiffness and reduced movement. In osteoarthritis, stiffness is often worse after rest and improves slightly with gentle movement. In rheumatoid arthritis, morning stiffness may last much longer.
4.2 Swelling and Warmth
Inflammatory forms of arthritis can cause swelling, warmth and tenderness around the joint. A person with rheumatoid arthritis may notice swollen knuckles and difficulty gripping a mug or turning a key.
4.3 Fatigue and General Illness
Inflammatory arthritis may also cause tiredness, malaise and sometimes weight loss. These wider symptoms are less typical of simple osteoarthritis and may suggest a systemic condition (Smolen et al., 2016).
4.4 Loss of Function
As arthritis progresses, everyday tasks may become difficult. Someone with hip osteoarthritis may struggle to put on shoes, while a person with hand arthritis may find writing or opening jars painful.
5.0 Prevention of Arthritis
5.1 Maintaining A Healthy Weight
One of the most effective ways to reduce the risk of osteoarthritis is to keep a healthy body weight. Even modest weight loss can reduce pressure on weight-bearing joints and lessen pain in people who already have knee arthritis (NICE, 2022).
5.2 Regular Physical Activity
Exercise helps strengthen muscles, support joints and maintain flexibility. Low-impact activities such as walking, swimming and cycling are particularly helpful. Strong thigh muscles, for example, can improve knee stability and reduce stress on the joint.
5.3 Avoiding Joint Injury
Using correct lifting techniques, wearing supportive footwear and taking care during sports can reduce long-term damage. Warm-up exercises and muscle conditioning are useful for injury prevention.
5.4 Stopping Smoking
Smoking is a recognised risk factor for rheumatoid arthritis and may also worsen disease severity. Avoiding smoking supports both joint and overall health (Smolen et al., 2016).
6.0 Management of Arthritis
6.1 Education and Self-Management
People benefit from understanding their condition and learning how to pace activity, manage flare-ups and stay active. Support groups and patient organisations can provide practical advice and reassurance. For example, learning to alternate activity with short rest periods can help someone with knee arthritis remain productive without worsening pain.
6.2 Exercise and Physiotherapy
Contrary to common belief, rest alone is not the best answer. Appropriate exercise is central to arthritis care. Physiotherapy can improve strength, balance and joint function, while occupational therapy may suggest aids for dressing, cooking or working (NICE, 2022).
6.3 Medicines
Treatment depends on the type of arthritis. For osteoarthritis, pain relief such as paracetamol or non-steroidal anti-inflammatory drugs may be used cautiously. Topical anti-inflammatory gels can also help some patients. In rheumatoid arthritis, disease-modifying antirheumatic drugs are essential because they reduce inflammation and prevent joint damage rather than simply masking pain (Smolen et al., 2016).
6.4 Lifestyle Measures
Heat packs, supportive footwear, balanced diet and adequate sleep may all help. In gout, dietary changes and medication to lower uric acid are important. In rheumatoid arthritis, prompt treatment is vital because early control leads to better long-term outcomes.
6.5 Surgery
When symptoms are severe and other treatments fail, joint replacement surgery may be considered, especially for hips or knees badly affected by osteoarthritis. Many patients experience major improvements in pain and mobility after successful surgery (Kumar and Clark, 2020).
Arthritis is a common but varied group of conditions that can affect people physically, emotionally and socially. Its causes include age, genetics, injury, excess weight and immune dysfunction, depending on the specific type. The main symptoms are pain, stiffness, swelling and reduced function, although inflammatory forms may also cause fatigue and wider health problems. While not all arthritis can be prevented, healthy weight, regular exercise, avoiding smoking and protecting joints can reduce risk. Effective management usually combines education, exercise, lifestyle changes and, where needed, medication or surgery. With early support and appropriate treatment, many people with arthritis can continue to lead active and fulfilling lives.
References
Firestein, G.S., Budd, R.C., Gabriel, S.E., McInnes, I.B. and O’Dell, J.R. (2021) Kelley and Firestein’s Textbook of Rheumatology. 11th edn. Philadelphia: Elsevier.
Hunter, D.J. and Bierma-Zeinstra, S. (2019) ‘Osteoarthritis’, The Lancet, 393(10182), pp. 1745–1759. Available at: https://doi.org/10.1016/S0140-6736(19)30417-9.
Kumar, P. and Clark, M. (2020) Kumar and Clark’s Clinical Medicine. 10th edn. Edinburgh: Elsevier.
McInnes, I.B. and Schett, G. (2017) ‘Pathogenetic insights from the treatment of rheumatoid arthritis’, The Lancet, 389(10086), pp. 2328–2337. Available at: https://doi.org/10.1016/S0140-6736(17)31472-1.
National Institute for Health and Care Excellence (NICE) (2022) Osteoarthritis in over 16s: diagnosis and management. Available at: https://www.nice.org.uk/guidance/ng226.
National Institute of Arthritis and Musculoskeletal and Skin Diseases (2023) Arthritis. Available at: https://www.niams.nih.gov/health-topics/arthritis.
NHS (2023) Arthritis. Available at: https://www.nhs.uk/conditions/arthritis/.
Safiri, S., Kolahi, A.-A., Smith, E., Hill, C., Bettampadi, D., Mansournia, M.A., Hoy, D., Ashrafi-Asgarabad, A., Moradi-Lakeh, M., Qorbani, M., Collins, G. and Woolf, A.D. (2020) ‘Global, regional and national burden of osteoarthritis 1990–2017’, Annals of the Rheumatic Diseases, 79(6), pp. 819–828. Available at: https://doi.org/10.1136/annrheumdis-2019-216515.
Smolen, J.S., Aletaha, D. and McInnes, I.B. (2016) ‘Rheumatoid arthritis’, The Lancet, 388(10055), pp. 2023–2038. Available at: https://doi.org/10.1016/S0140-6736(16)30173-8.
Versus Arthritis (2024) Arthritis. Available at: https://www.versusarthritis.org/.
World Health Organization (2023) Musculoskeletal health. Available at: https://www.who.int/news-room/fact-sheets/detail/musculoskeletal-conditions.